Utilising Digital Technology to Support Treatment of Alcohol Misuse During the COVID-19 Pandemic
The COVID-19 pandemic is a unique situation. The implementation of social distancing and lockdown measures means that daily life has been completely redefined for the majority of the population, with many people left feeling isolated and facing new challenges. These include unemployment, increased or changed caring responsibilities, financial difficulties and psychological distress.
Approximately 30 million people in Great Britain reported drinking alcohol and more than 7,500 alcohol-specific deaths were registered in the United Kingdom (UK) in 2018. As social distancing and lockdown measures remain in place, the effects of long-term isolation on alcohol use are not yet clear. So far, the first lockdown appears to have changed drinking habits in the UK at both ends of the spectrum, with 21% drinking more frequently, while just 9% reduced drinking and 55% stayed the same. This varied with factors such as age, occupational status and socio-economic group. For example, 33% of working people, versus 20% of non-working people, agreed to drinking more. Alcohol consumption has also increased with 13% of drinkers, and 38% of heavy drinkers (seven or more UK units), reporting an increase the average number of units consumed since the beginning of the first lockdown.
Alcohol misuse is associated with several negative consequences relating to health, economic and social factors, at both an individual and societal level. It has many psychiatric comorbidities, including anxiety disorders, however the causal direction of this relationship is almost impossible to determine. Alcohol is often used as a coping mechanism for stress. UK based research has shown that alcohol misuse has been exacerbated during the pandemic, with 19% of drinkers reporting drinking due to stress and anxiety attributed to the first nationwide lockdown measures.
The UK Armed Forces, including ex-serving personnel (referred to herein as veterans), are more likely to experience hazardous and harmful alcohol use when compared to the general population. These higher rates of alcohol misuse are also exhibited by veterans who seek help for mental health difficulties. Alcohol is often used as a coping mechanism to deal with the stresses of a military career, but it is also associated with the transition back to civilian life which many find stressful. Among the veteran population alcohol misuse is often experienced comorbid with post-traumatic stress disorder (PTSD). In one recent study by a UK veteran's mental health charity, approximately 30% of veterans reported that their alcohol symptoms have been exacerbated by the pandemic.
Managing alcohol consumption is an important step in protecting both physical and psychological well-being, especially because it significantly increases the risk of contracting lung infections, including COVID-19. A variety of effective intervention techniques are available to support, manage or reduce alcohol misuse, including self-help groups, cognitive behavioural therapy and mobile apps (for example, Drink Less and Drinkaware). Brief interventions are the most widely used intervention in the UK, aiming to recognise risk and reduce consumption. Treating alcohol misuse is challenging due to several barriers including the perceived stigma of seeking support and the accessibility and availability of treatment. Can digital technology help to overcome some of these barriers? We believe so.
With a growing strain on healthcare services, digital technologies are becoming increasingly popular in healthcare delivery and monitoring. The nature of the COVID-19 pandemic has forced a rapid, large-scale implementation of digital technology within healthcare contexts. Although digital care may risk depersonalising the patient-professional experience, it allows for the provision of care when face-to-face contact is not viable.
Smartphone-based interventions offer a diverse range of treatment possibilities and have several advantages over traditional interventions. They can be used anywhere and at any time, helping to target ‘hard to reach’ populations and those underserved by current treatment options. Apps are accessed at the user’s discretion, providing control and reducing any perceived power imbalance with professionals. Increasing anonymity can reduce the perceived stigma associated with seeking help for alcohol misuse. However, smartphone apps may have difficulty with levels of engagement and high attrition rates.
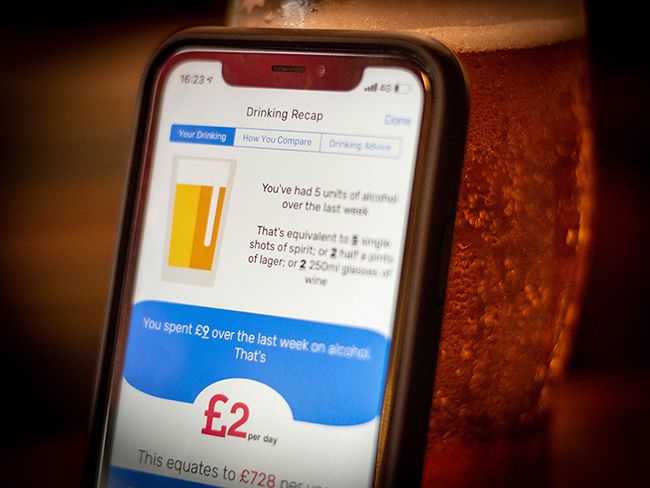
We are currently trialing a new smartphone-based alcohol reduction intervention, Drinks:Ration (formerly InDEx), funded by the Forces in Mind Trust. The app has been designed to reduce alcohol consumption among veterans who drink at a hazardous or harmful level and are receiving, or have received, support for mental health symptoms in a clinical setting. We hope that Drinks:Ration will be an effective tool to support this population, particularly at present while the impact of the COVID-19 pandemic remains unclear.
Although digital technologies have been adopted at great speed due to COVID-19, we believe that they will become a long-lasting positive consequence of the pandemic. The research community should actively seek, where possible, to share data collected and tools used for a wider societal benefit. Using digital technology in healthcare, including alcohol services, has displayed undeniable strengths and holds great potential to continue as part of routine care. Smartphone-based interventions allow for rapid advancement and development at a rate that could not be matched by traditional approaches. Digital technology is beginning to break down the barriers associated with seeking support for alcohol misuse, something that healthcare professionals cannot overcome using traditional methods.
Header photo by Guillermo Nolasco on Unsplash.
